Subconjunctival orbital fat prolapse is a rarely reported, benign condition. Most patients present for evaluation due to cosmetic concerns or to rule out potential for malignancy.
Orbital fat occupies the space surrounding the eye muscles and the eye—as a protective cushion for the eye. The orbital fat is comprised of two compartments: intraconal and extraconal. Orbital fat may be prolapsed or displaced secondary to aging, trauma or surgery. With extraconal fat prolapse, the orbital fat migrates beyond the orbital septum and results in lower lid festoons (commonly called bags under the eyes). When intraconal fat is displaced through Tenon’s capsule (tissue that surrounds the eye muscles that acts as a pully), it can be visualized in the subconjunctival space like the photo below.
Subconjunctival orbital fat is most commonly seen in elderly males as a result of age-related weakening of Tenon’s capsule. This finding may be unilateral or bilateral, but in bilateral cases it is often asymmetric. Subconjunctival herniated orbital fat presents as a soft, mobile, yellow mass with superficial vasculature.This mass is most often seen in the supper/outer quadrant and can be
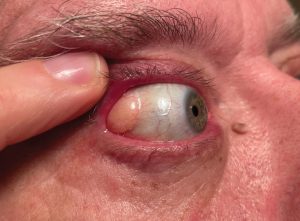
indented with a cotton tip applicator. Prolapsed orbital fat will become more prominent with pressure applied to the globe or with downward movement of the eye. Patients with subconjunctival herniated orbital fat are typically asymptomatic; however, patients may report mild irritation and tearing.
Most often, subconjunctival herniated orbital fat can be differentiated from other orbital tumors on clinical exam. But in difficult cases, a biopsy may be required to make a definitive diagnosis.
MRI or CT-scan also clearly demonstrate prolapsed orbital fat, but are indicated only when a diagnosis cannot be made based on clinical exam. With MRI or CT-Scan, subconjunctival orbital fat prolapse is continuous with the intraconal fat, unlike many other orbital lesions.
Treatment of subconjunctival orbital fat prolapse typically involves observation. In some cases, a patient may elect to have the mass removed due to symptoms, cosmetic concerns or suspicion for malignancy. Most often, prolapsed fat is accessed through a trans-conjunctival incision. Orbital fat is typically resected and the incision is then closed with sutures or fibrin glue.This procedure is performed on an outpatient basis and involves local anesthesia. Some surgeons prefer to reposition the orbital fat rather than resect it; however, resection is still the most common approach. Risks of surgical resection include infection, lacrimal gland damage and retrobulbar hemorrhage. Fortunately, this procedure has a high success rate and risk of recurrence is low.
